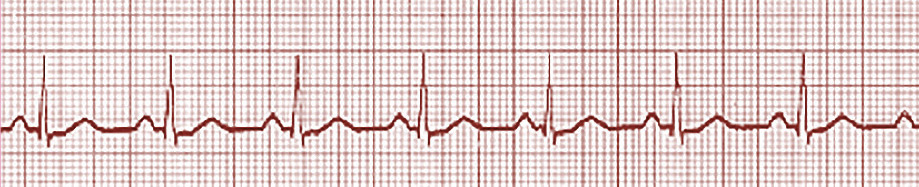
See Figure 7.17 for an image of sinus tachycardia.Ī sinus rhythm with a slower rate than normal range (i.e., less than 60 in an adult) is called a sinus bradycardia. 
However, sinus tachycardia can also be caused by conditions such as hypovolemia, anemia, fever/infection, decreased oxygenation, cardiac conditions, and some medications, requiring nursing action depending upon the cause. Sinus tachycardia is commonly caused by stress, exercise, alcohol, caffeine, and tobacco and can be resolved by addressing these causes. See Figure 7.16 for an image of normal sinus rhythm.Ī sinus rhythm faster than a normal rate (i.e., greater than 100 in adults) is called a sinus tachycardia. All components of the ECG waveform are within normal limits. Normal sinus rhythm (NSR) originates from the sinus node and describes the characteristic rhythm of a healthy human heart. Characteristics and treatment of sinus rhythms are summarized in Table 7.4a at the end of this subsection. When the rhythm is regular but there is an abnormal rate, it is called “sinus arrhythmia.” Sinus arrhythmias include sinus tachycardia and sinus bradycardia. Sinus rhythm is a regular rhythm, but the rate varies depending on autonomic nervous system regulation of the sinus node. A table summarizing the ECG images discussed in this chapter can be found in the “ Appendix of Rhythm Strips.” Sinus Rhythms The characteristics of each of these types of rhythms and blocks are further discussed in the following sections. Additionally, heart blocks refer to blocks in the normal pathway of electrical conduction through the heart and can be categorized as sinus node, atrioventricular (AV) node, or bundle branch blocks. Cardioversion and defibrillation are further discussed in the “ Cardioversion and Defibrillation” section of this chapter.ĮCG patterns are generally classified into three categories depending on whether the signal originates from the SA node (i.e, sinus rhythms), the atria (i.e., atrial rhythms), or the ventricles (i.e., ventricular rhythms). Medical treatments for symptomatic dysrhythmias can include antidysrhythmic medications, cardioversion, defibrillation, and/or implantation of medical devices such as pacemakers and implantable cardioverter defibrillators (ICDs). The nurse must be aware of which rhythms require emergency assistance. Some dysrhythmias can quickly lead to cardiac arrest, such as ventricular tachycardia, ventricular fibrillation, and third-degree heart block. 
When an ECG demonstrates new abnormal findings, the nurse must immediately assess the client for signs of decreased cardiac output and respond appropriately. If the ventricles become unable to effectively pump blood to the rest of the body due to altered electrical signals, signs and symptoms of decreased cardiac output occur, such as decreased blood pressure and pulses, prolonged capillary refill, chest pain, shortness of breath, dizziness, confusion, or loss of consciousness. Recall that the electrical conduction system stimulates the mechanical pumping action of the heart. Early and accurate identification of ECG patterns, assessment of the client’s clinical presentation, and knowledge of the agency’s policies and procedures regarding treatment will ensure clients receive optimal care. Some dysrhythmias can significantly affect the client’s clinical status and require rapid nurse response. Abnormal ECG waveforms indicate dysrhythmias (also referred to as arrhythmias).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
